WHO A health worker in Motema Pembe area prepares for a household decontamination in Mbandaka, Democratic Republic of the Congo.
A global population weary of the chaos caused by COVID-19 pandemic had to contend with a new, highly transmissible variant at the beginning of the year: Omicron.
Omicron and on
This latest version swept across Europe, leading to record weekly case numbers, although the number of deaths was relatively low, compared to previous outbreaks.
And, although many countries began to relax lockdown and other restrictions on movements, the World Health Organization (WHO) pointed out that the disease is still a threat: by August, one million COVID-19 related deaths had been recorded.
At the agency’s World Health Assembly in May – the first to be held in-person since a pre-pandemic 2019 – the WHO chief, Tedros Adhanom Ghebreyesus, urged countries not to lower their guard.
“Is COVID-19 over? No, it’s most certainly not over. I know that’s not the message you want to hear, and it’s definitely not the message I want to deliver”, he told delegates.

UNICEF/Laxmi Prasad Ngakhusi A health worker delivers COVID-19 vaccines, donated through the COVAX Facility, to a health post in Nepal
A billion COVAX jabs delivered
Since early on in the pandemic, the WHO consistently called out the unequal distribution of vaccines and treatments for COVID-19, urging for more to be done for those living in developing countries: the UN-backed COVAX facility, a multilateral initiative to provide equal vaccine access to all, reached a major milestone in January, when the billionth jab was recorded in Rwanda.
COVAX has undoubtedly saved many lives but, by March, Tedros was warning that a third of the world’s population had still not received a single dose of COVID-19 vaccine, including a shocking 83 per cent of all Africans.
This lack of equity was still a problem in November, when a WHO report confirmed that lower-income countries consistently struggle to access essential inoculations in demand by wealthier countries.
“This is not acceptable to me, and it should not be acceptable to anyone”, said Tedros. “If the world’s rich are enjoying the benefits of high vaccine coverage, why shouldn’t the world’s poor? Are some lives worth more than others?”
AIDS eradication targets off-track
In 2021, there were 1.5 million new HIV infections and 650,000 AIDS-related deaths. UN Member States had demonstrated their commitment to ending the virus by the end of the decade, with the signing of a political declaration at the General Assembly in 2021, but it was clear this year that swifter action would be needed, if that goal is to be met.
A July report showed a slowing of the rate at which HIV infections decline, to 3.6 per cent between 2020 and 2021, the smallest annual decline in new HIV infections since 2016. The pandemic has thrived as COVID-19, and other global crises put a strain on resources, to the detriment of HIV programmes.
On World AIDS Day in November, UN chief António Guterres declared that the 2030 goal is off-track, and noted the ongoing discrimination, stigma, and exclusion, many people living with HIV still face.
This year saw encouraging developments in drug treatments: in March, the first injection to offer long-lasting protection against HIV was rolled out in South Africa and Brazil, as an alternative to daily medication.
WHO recommended the use of the drug, Cabotegravir, which only needs to be injected six times a year, for people at substantial risk of HIV infection. In July, the UN reached a deal with the company that developed the drug, to allow low-cost, generic formulations to be produced in less-developed countries, a move that could potentially save many lives.

© UNICEF/Thomas Nybo Ebola treatment centre in Beni, Democratic Republic of the Congo.
DRC and Uganda hit by Ebola
In April, health workers were mobilized to fight an outbreak of the deadly Ebola virus in the Democratic Republic of Congo (DRC), the sixth recorded outbreak in just four years. “With effective vaccines at hand and the experience of DRC health workers in Ebola response, we can quickly change the course of this outbreak for the better,” said Dr Matshidiso Moeti, the WHO’s Regional Director for Africa.
An outbreak was also reported in neighbouring Uganda in August, following six suspicious deaths in the central Mubende district, a region with gold mines, which attract workers from many parts of Uganda, and other countries.
The following month, the WHO scaled up response efforts, delivering medical supplies, providing logistics, and deploying staff to support the Ugandan authorities in halting the spread of the virus.
By mid-November, 141 cases and 55 deaths had been confirmed, and the UN health agency reassured that it was working closely with the Ugandan authorities to speed up the development of new vaccines.
Cholera returns to Haiti, threatens Middle East
As the security situation in Haiti continued to degrade, cholera made an unwelcome return to the troubled country in October, linked to a degraded sanitation system and lawlessness, which made it harder for sufferers to seek treatment.
The situation was exacerbated by gangs blockading Haiti’s main fuel terminal. That led to a deadly fuel shortage that forced many hospitals and health centres to close and affected water distribution.
The UN children’s agency, UNICEF, declared in November that youngsters account for around 40 per cent of cases in Haiti, and appealed for $27.5 million, to save lives from the disease.
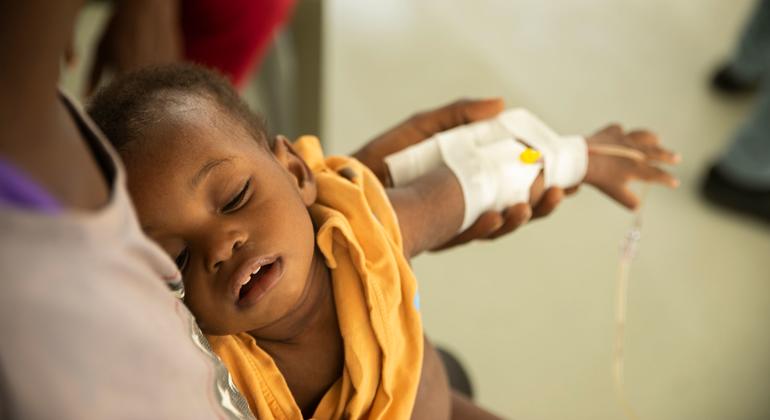
© UNICEF/Odelyn Joseph A young child is treated for cholera at a hospital in Port-au-Prince, Haiti.
Haiti was far from the only country to be affected by the bacterial disease: an outbreak in the Syrian city of Aleppo in September, was attributed to people drinking unsafe water from the Euphrates River and using contaminated water to irrigate crops, resulting in food contamination. An outbreak in Lebanon, the first in thirty years, spread through the country in November. WHO declared that the situation was fragile, with Lebanon facing a prolonged crisis, and limited access to clean water and proper sanitation across the country.
WHO data released in December, pointed to cases of infection in around 30 countries, whereas in the previous five years, fewer than 20 countries reported infections.
“The situation is quite unprecedented, for not only we are seeing more outbreaks, but these outbreaks are larger and more deadly than the ones we have seen in past years,” said Dr. Barboza, WHO Team Lead for Cholera and Epidemic Diarrhoeal Diseases.
Mr. Barboza said that, whilst conflict and mass displacement continue to be major factors in allowing cholera to spread, the climate crisis is playing a direct role in the growing number of simultaneously occurring outbreaks.
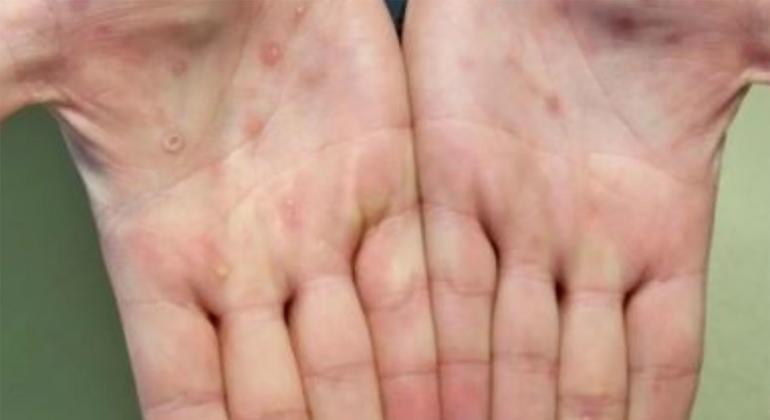
© CDC Monkeypox lesions often appear on the palms of hands
Mpox: a new health emergency
For many people, monkeypox was a previously unknown word to learn in 2022, although the disease has been associated with illness in humans since 1970. Monkeypox, renamed mpox by WHO, occurs primarily in tropical rainforest areas of Central and West Africa, but outbreaks began to emerge in other parts of the world this year.
In May, WHO was at pains to allay concerns that the outbreak would resemble the COVID-19 pandemic, noting that most of those infected recover, without treatment, in a number of weeks.
However, with global cases growing, WHO declared in July that mpox qualified as a “global health emergency of international concern”. Tedros stressed that, because the virus was concentrated among men who have sex with men, especially those with multiple sexual partners, the outbreak could be stopped, “with the right strategies in the right groups”.
A senior WHO official observed, in August, that the international community only became interested in mpox once infections grew in the developed world.
Assistant Director-General for Emergencies, Ibrahima Soce, said in August that “we have been working on mpox in Africa for several years, but nobody was interested”.
In late November WHO announced that they would henceforth refer to Monkeypox as mpox, citing reports of racist and stigmatizing language surrounding the name of the disease.
By December, more than 80,000 cases were reported in 110 countries, with 55 deaths.

GAVI Malaria vaccine at a health facitlity in Kenya
Major malaria breakthrough
Hopes of an end to malaria were raised in August, when UNICEF announced that the pharmaceutical giant GSK had been awarded a $170 million contract to produce the first world’s first malaria vaccine.
Malaria remains one of the biggest killers of children under five: in 2020, nearly half a million boys and girls died from the disease in Africa alone, a rate of one death every minute.
“This is a giant step forward in our collective efforts to save children’s lives and reduce the burden of malaria as part of wider malaria prevention and control programmes”, said Etleva Kadilli, Director of UNICEF’s Supply Division.
Plans are already underway to boost production, including through technology transfer, UNICEF added, “so that every child at risk will one day have the opportunity to be immunized against this killer disease”.

